
Pain in Ayurveda: Vata’s Domain
You have done the scans. The blood work came back normal. The MRI showed “mild degenerative changes, consistent with age.” And yet your body is screaming. You know the pain is real — it wakes you at 3 AM, it steals your concentration, it has quietly rearranged your entire life. But somewhere along the way, someone shrugged and said: “We can’t find anything wrong.” Ayurveda would never say that. Not because it ignores diagnostics, but because it starts from a fundamentally different premise about what pain is. Charaka Samhita (Sutra Sthana 12.8) makes a statement that sounds bold until you understand its logic: “Naasti Vata-rite shulam” — there is no pain without Vata. This does not mean Pitta and Kapha never contribute. It means the sensation of pain itself — the sharp, throbbing, aching, shooting experience called Shula — is always a function of Vata. Other doshas may create the conditions — Pitta inflames, Kapha congests — but the pain you actually feel is Vata carrying that signal through the nervous system. This single insight shifts the question from “what is hurting?” to “why is Vata behaving this way?” And that changes everything.
Pain happens through two primary mechanisms in Ayurvedic physiology, and knowing which one is driving your pain changes the entire approach. The first is Avarana — obstruction. Think of a garden hose with a kink in it: water pressure builds behind the kink, the hose swells, and nothing flows past the blockage. When something blocks Vata’s natural movement through a channel — Ama deposits, tissue swelling, postural compression — Vata builds up behind the obstruction. The pressure creates pain. This is the mechanism behind joint stiffness after prolonged sitting, the ache that develops when circulation is impaired, and the deep pain of organ congestion. The second mechanism is Dhatukshaya — tissue depletion. Imagine the walls of that same hose becoming thin and brittle: now even normal water pressure causes pain because the structure itself cannot hold. When tissues are inadequately nourished, Vata occupies the empty space. The result is the kind of pain that comes with ageing, with chronic illness, with prolonged nutritional deficiency — a pain that feels deep, empty, and worse with activity. Here is the crucial part that most people miss: these two mechanisms require opposite approaches. Treating an obstruction problem with nourishment makes it worse. Treating a depletion problem with clearing makes it worse. This is why the same chronic pain responds brilliantly to one approach and terribly to another — and why so many people cycle through treatments that “should work” but do not.
Vataja pain — pain driven primarily by Vata — has a signature so distinctive that many people recognise it immediately once it is described. It is dry rather than inflamed. It moves around rather than staying fixed in one place. It is variable in intensity, sometimes severe and sometimes barely noticeable, often changing with the weather, the time of day, or your emotional state. It worsens with cold, wind, movement, and irregularity. It improves with warmth, oil, rest, and routine. If you have ever noticed that your pain flares on cold, windy days, eases when you take a warm bath, and seems to vanish on holiday only to return the moment you resume your routine — you are looking at a Vata-dominant pain pattern. The connection to stress is not coincidental: Vata governs the nervous system, and emotional turbulence directly aggravates it.
Ama-associated pain is fundamentally different, and confusing it with Vataja pain is one of the most common reasons people feel that “nothing works” for their chronic pain. Ama — metabolic waste that has not been fully processed by Agni — creates pain that is heavy, fixed, and worse in the morning. Where Vata pain feels empty and dry, Ama pain feels congested and stuck. It does not move around. It settles in a specific location and stays there. The affected area may feel heavy, stiff, and swollen rather than sharp and shooting. Here is a practical test that Ayurvedic practitioners use: does your pain feel better or worse after eating? Vata pain often temporarily improves after a warm meal (nourishment calms Vata). Ama pain often worsens after eating (digestion mobilises toxins). This single observation can point toward the dominant mechanism.
Chronic pain is different from acute pain in a way that Ayurveda understood long before modern pain science arrived at the same conclusion. Acute pain is a signal — something is wrong right now, pay attention. Chronic pain is a pattern — the signal has become self-sustaining, the nervous system has reorganised around pain, and the original cause may no longer be the driving factor. Charaka describes this progression explicitly (Chikitsa Sthana 28): Vata first accumulates, then aggravates, then spreads into weakened tissues where it “takes up residence” (Sthana Samshraya). Once Vata is lodged, the imbalance perpetuates itself — the channels adapt to obstruction, the tissues adapt to depletion. This is why people with long-standing pain conditions often say their pain has “a life of its own.” It does. The system has settled into a new, dysfunctional equilibrium, and simply removing the original trigger is no longer sufficient.
Here is what makes this understanding so important for anyone who has been told their pain is “all in their head”: Ayurveda has never separated the two. Vata governs both the nervous system and the mind. When Vata is aggravated, it does not choose between physical symptoms and psychological ones — it creates both simultaneously. The anxiety that accompanies chronic pain is not a separate condition or a sign of weakness. It is Vata doing what Vata does when disturbed: creating instability everywhere it flows. Modern pain neuroscience now calls this the biopsychosocial model of pain — the recognition that pain is never purely physical or purely psychological, but an integrated experience. Ayurveda never needed to arrive at that conclusion because it never made the separation in the first place.
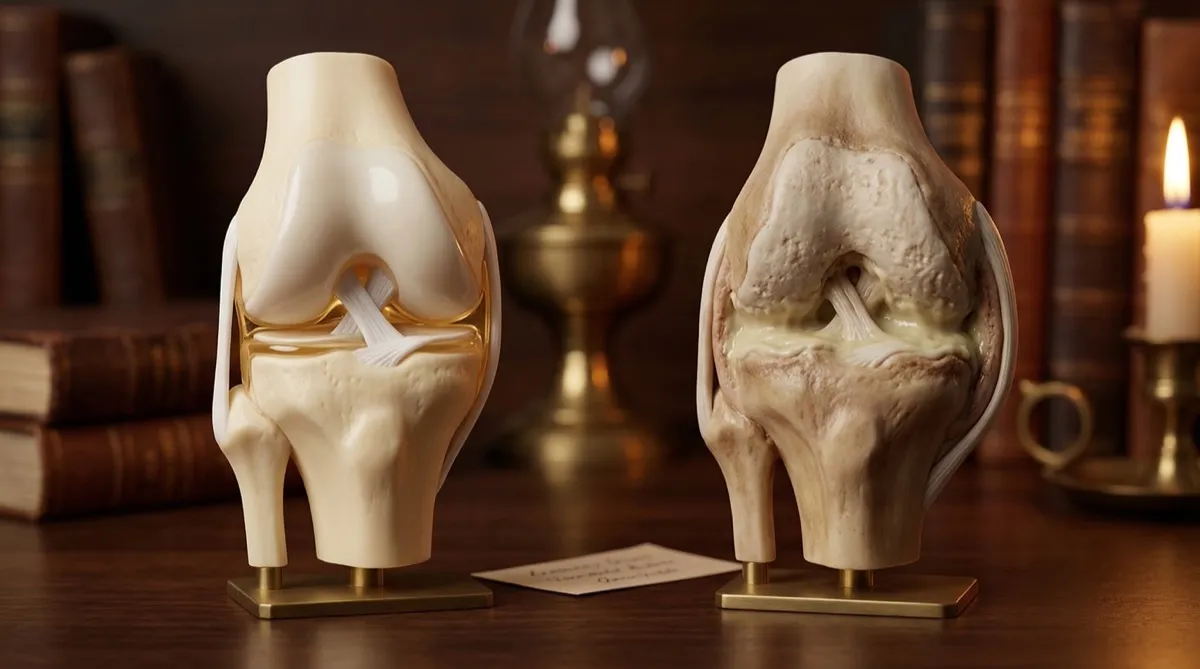
Here is something that should reframe how you think about chronic pain entirely: the brain can learn pain. Chronic pain is not just tissue damage that persists — it is the nervous system literally rewiring itself to produce pain more efficiently, even after the original injury has healed. Neuroscientists call this central sensitisation. The pain pathways become so well-practised that they fire with less and less provocation — eventually firing on their own, producing genuine, agonising pain in tissues that are structurally intact. This is why an MRI can look perfectly normal while the person is in unbearable pain. The problem is no longer in the knee or the back. It is in the nervous system itself — in the Vata-governed pathways that have settled into a dysfunctional pattern. Ayurveda described this process as Vata taking up residence (Sthana Samshraya) in weakened tissues and channels, where it perpetuates itself independently of the original trigger. Two frameworks, two millennia apart, describing the same phenomenon: pain that has become self-sustaining.
Did You Know?
Madhava Nidana, written in the 7th century CE, devoted an entire chapter (Chapter 25) to Amavata — a condition presenting with morning stiffness, joint swelling, migratory pain, fatigue, and digestive weakness. The text describes the exact clinical progression: weakened Agni produces Ama, Ama combines with Vata in the gut, and this toxic combination migrates into joints where it causes swelling, pain, and restricted movement. Modern rheumatology identifies rheumatoid arthritis as an autoimmune condition where gut-derived inflammatory molecules trigger joint inflammation — a gut-joint axis that was formally proposed in the Lancet only in 2018. The Madhava Nidana described the clinical presentation, the progression pattern, the gut origin, and the migratory nature of the condition 1,300 years before the gut-joint connection became a research frontier in Western medicine. It is one of the most clinically precise descriptions in all of classical Ayurvedic literature.
Ama and Pain: The Inflammation Connection
If you have ever wondered why your pain is worst first thing in the morning and gradually eases as the day progresses, Ama is likely the reason. Ama is one of the most clinically important concepts in Ayurveda, and nowhere is its relevance more apparent than in chronic pain. Ama is the product of incomplete digestion — not just of food, but of any input that the body’s Agni fails to fully process. When Agni is weak, food is not completely broken down. The partially processed material — heavy, sticky, and toxic in nature — enters the circulation and lodges wherever it finds a vulnerable site: joints, muscles, channels, spaces between tissues. Overnight, while the body is still, Ama settles and consolidates. By morning, the affected areas are at their stiffest. Movement and warmth gradually dislodge some of it, which is why morning stiffness that improves as you “get going” is the hallmark of Ama-driven pain.
When Ama combines with aggravated Vata, the result is what Ayurveda calls Amavata — a condition described in Madhava Nidana (Chapter 25) with such clinical precision that it reads like a modern rheumatology textbook written twelve centuries early. Amavata presents as pain with stiffness, swelling, heaviness, and a characteristic worsening in the morning or after periods of rest. The pain is both fixed (because of Ama’s heavy, sticky nature) and eventually spreading (because Vata carries Ama to new locations). Madhava Nidana traces the exact progression: first the weakening of Agni, then the formation of Ama, then its combination with Vata in the gut, and finally its migration into joints and tissues throughout the body. The text even notes that the condition tends to affect multiple joints sequentially — an observation that modern medicine calls “migratory polyarthritis.”
This understanding explains why simply “taking something for pain” does not work long-term for many chronic pain conditions. If the underlying Ama is not addressed, pain relief is temporary. The Ama remains in the tissues, continuing to obstruct channels and provoke Vata. As soon as the pain-relieving intervention wears off, the pain returns — often worse than before, because the Ama has continued to accumulate while the symptom was masked. This is the Ayurvedic explanation for the common clinical observation that chronic pain patients often need escalating doses of pain management: the symptom is being suppressed, but the cause is progressing.
The connection to weak Agni makes this a systemic issue, not a local one. A person with chronic pain in their knee does not simply have a knee problem — they have an Agni problem that is manifesting in the knee. Until Agni is strengthened and Ama production is reduced at its source, local treatment provides only temporary relief. This is why Ayurvedic approaches to chronic pain always include attention to digestion, dietary modification, and Agni restoration — even when the pain seems entirely unrelated to the digestive system. For a deeper understanding of this digestive foundation, see our article on Agni and Digestion.
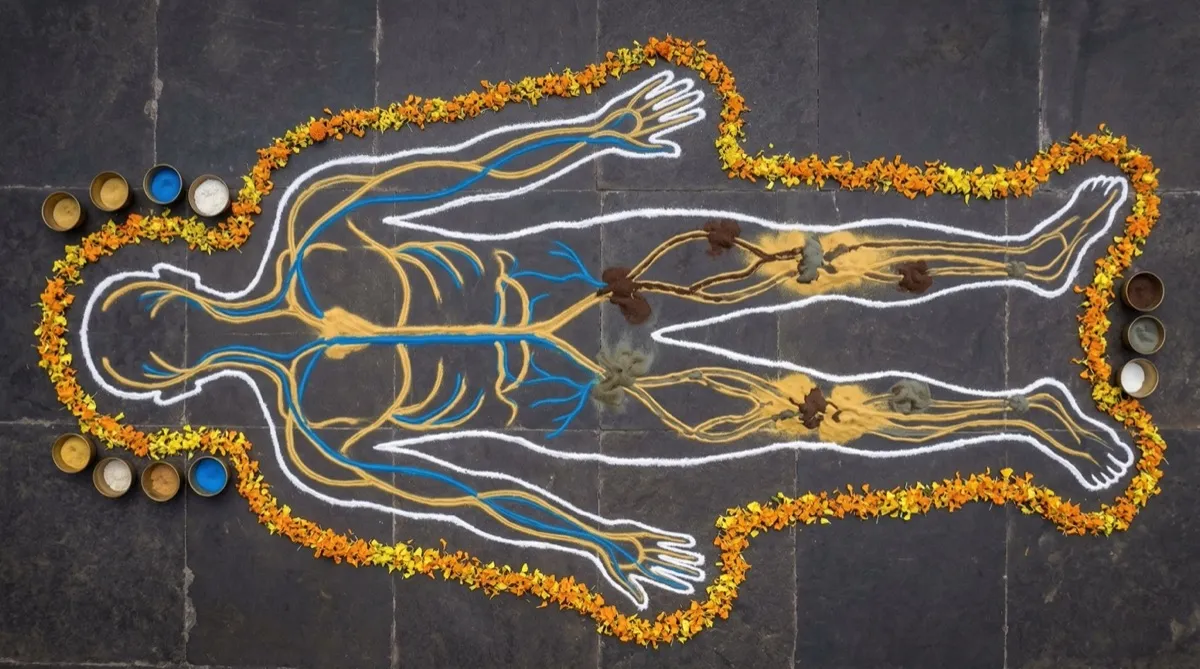
The Channel Theory: Why Pain Shows Up Where It Does
Here is a question that haunts people with chronic pain: why here? You have two knees, but only the left one hurts. You have an entire spine, but the pain lives only between L4 and L5. And then, maddeningly, the knee finally settles down — and your shoulder starts. Your doctor says these are “unrelated.” Ayurveda says they are intimately connected. The answer lies in the theory of Srotas — the channels through which all physiological processes flow — and Marma — the vital junction points where channels converge. Sushruta (Sharira Sthana 9) describes the body not as a collection of separate parts but as an interconnected river system. Pain does not randomly land — it follows the current.
Think of it this way: a city has a water supply network with thousands of pipes. A blockage in a main pipe does not cause problems everywhere equally — it causes problems in whichever homes and buildings are downstream of that particular blockage. The body’s Srotas work similarly. Each channel carries specific substances to specific tissues. When a channel becomes blocked — by Ama, by doshic aggravation, by trauma, by compression — the tissue served by that channel begins to starve. Vata accumulates at the site of obstruction. Pain manifests. The location of the pain tells the practitioner which Srotas are involved, and this in turn reveals the deeper pattern of imbalance. It is not a guess — it is a diagnostic map.
Different Srotas involvement creates distinctly different pain patterns. Asthivaha Srotas — the channels that nourish bone tissue — when compromised, produce deep, gnawing bone pain that worsens with pressure and feels like it originates from within the structure itself. Mamsavaha Srotas — the channels nourishing muscle tissue — when blocked, create the aching, cramping, heavy muscular pain that many people describe as “tightness” or “knots.” Majjavaha Srotas — the channels serving nerve tissue and marrow — when disturbed, generate the sharp, shooting, burning nerve pain that radiates along pathways and often comes with tingling or numbness.
This channel-based framework explains something that puzzles many pain patients: why pain moves. A person may have lower back pain for months, then the back improves and the knee begins to hurt, then the knee settles and shoulder pain appears. From a conventional perspective, these may seem like unrelated problems. From the Srotas perspective, they are manifestations of the same underlying imbalance — Vata aggravation with Ama — expressing through whichever channels are most vulnerable at a given time. The pain is not moving randomly. It is following Vata’s nature: mobile, unpredictable, seeking out the weakest points in the system.
Marma points add another layer to this understanding. These are vital junction points where muscles, bones, joints, tendons, blood vessels, and nerves converge. Classical texts describe 107 Marma points across the body. When Vata and Ama accumulate at a Marma point, the pain can be disproportionately severe relative to the apparent cause, because the Marma serves as a nexus for multiple channels. Pain at a Marma point often affects function beyond the immediate area — a Marma involvement in the wrist may affect grip strength, sensation in the fingers, and mobility throughout the forearm.

Dosha-Specific Pain Patterns
Recognising the doshic quality of pain is not an academic exercise — it determines the entire approach to addressing it, and getting it wrong can make your pain worse. Each dosha creates a pain signature so distinctive that an experienced practitioner can often identify the dominant dosha simply from how the patient describes their pain. Your Prakriti (constitutional type) also matters here: you are most vulnerable to pain patterns that match your dominant dosha. A Vata-predominant person is more susceptible to Vataja pain; a Pitta-predominant person to Pitta-type pain. These patterns are not always pure — chronic conditions often involve mixed patterns — but understanding the individual contributions of each dosha provides the framework for effective intervention.
Vata pain is the most common type in chronic conditions, particularly in the elderly (Ayurveda considers the entire post-60 phase of life to be Vata-dominant) and in people living irregular, high-stress lifestyles. Its qualities mirror Vata’s own nature: dry, light, cold, mobile, and subtle. Vata pain is shooting, piercing, or throbbing. It moves from place to place. It varies in intensity — severe one day, nearly absent the next. It worsens dramatically with cold weather, wind, excessive movement, irregular eating, lack of sleep, and emotional stress. It improves with warmth, oil application, rest, regularity, and calm surroundings. The affected area often feels dry and cold to the touch. Cracking or popping sounds in the joints are common. Vata pain is frequently accompanied by stiffness that improves with gentle movement but worsens with overexertion. If this description resonates, pay attention to this detail: Vata pain often responds dramatically to simple lifestyle regularity — eating and sleeping at consistent times — before any other intervention is even needed.
Pitta pain has an entirely different character. It is burning, sharp, and inflamed. Where Vata pain feels empty, Pitta pain feels hot and full. The affected area is often red, warm to the touch, and visibly swollen. Pitta pain does not move around — it stays precisely where the inflammation is concentrated. It worsens with heat, sun exposure, anger, frustration, spicy food, and alcohol. It improves with cooling applications, calm mental states, and anti-inflammatory dietary choices. Pitta pain tends to be most intense during the Pitta time of day (10 AM to 2 PM) and during summer months. The associated emotions are irritability and impatience — the person in Pitta pain wants the pain gone now and is frustrated by its persistence.
Kapha pain is the most deceptive because it can feel less acute than Vata or Pitta pain, leading patients to underestimate its significance. Kapha pain is dull, heavy, and aching. There is often visible swelling — not the hot, red swelling of Pitta, but a cool, pale, boggy swelling. The affected area feels heavy and waterlogged. Kapha pain is worst in the morning and during cold, damp weather. It improves as the day progresses and with warmth, light exercise, and dry conditions. Kapha pain settles in one place and stays there with remarkable persistence. It is the pain of congestion, of excess fluid in tissues, of channels clogged not by the dry obstruction of Vata but by the heavy, wet accumulation of Kapha.
In chronic conditions, mixed patterns are the norm rather than the exception. Vata-Pitta pain combines the mobility of Vata with the inflammation of Pitta — pain that moves and burns. Vata-Kapha pain combines dryness and depletion with congestion — pain that is both empty and heavy, a confusing combination that responds poorly to simple approaches. Pitta-Kapha pain combines heat with congestion — inflamed, swollen, heavy, and stubborn. Understanding which doshas are involved and in what proportion is essential because the approach for each is different, and addressing the wrong dosha can make the condition worse.
Did You Know?
In 2019, the International Association for the Study of Pain (IASP) officially redefined pain for the first time in 41 years. The new definition added a revolutionary note: “Pain is always a personal experience that is influenced to varying degrees by biological, psychological, and social factors.” They also explicitly stated that a person’s report of pain should be accepted — even when no tissue damage can be found. Charaka Samhita made an almost identical argument roughly 2,000 years earlier. Charaka (Sutra Sthana 20.11) lists 80 distinct disorders caused by Vata alone — Vata Nanatmaja Vikara — classifying each not just by body location but by the quality of the pain, its time pattern, and the factors that worsen or relieve it. This is pain phenotyping — a concept modern medicine only formalised in the 2010s. The idea that the same knee pain in two people might need completely different approaches based on whether it is dry-and-moving or heavy-and-fixed? That was not a modern breakthrough. It was the starting point of Ayurvedic pain care.

The Ayurvedic Approach: Beyond Pain Relief
If you have lived with chronic pain for years, you have probably tried many things — and you may have noticed that relief, when it comes, is always temporary. The Ayurvedic approach begins with understanding why: most pain management addresses the last link in a long chain of causation. The root of chronic pain is almost never in the location where pain is felt. It is in the combination of weak Agni producing Ama, aggravated Vata carrying that Ama into vulnerable channels, and depleted tissues unable to maintain their integrity. Sushruta Samhita (Sharira Sthana 4) describes pain as a downstream event — the final expression of a process that began silently, often months or years before the pain appeared. Until that upstream process is addressed, downstream relief will always be temporary.
Strengthening Agni is the first priority. If Agni remains weak, Ama continues to form regardless of what else is done. Dietary modifications form the foundation: warm, freshly cooked, easily digestible food eaten at regular times. Cold, raw, heavy, and processed food is reduced or eliminated — not as a permanent restriction, but as a therapeutic intervention until Agni recovers. Irregular eating patterns are corrected because irregularity itself aggravates Vata, which in turn destabilises Agni. The goal is to stop the production of new Ama at its source while the existing Ama is gradually cleared from the tissues. For a deeper understanding of why Agni is so central, see our article on Agni and Digestion.
Pacifying Vata is the second pillar, and this is where people living with chronic pain often experience the most tangible shifts. Since Vata is the vehicle that carries pain, calming Vata reduces pain directly — not by numbing the signal, but by reducing the force that generates and transmits it. Charaka (Chikitsa Sthana 28.75–80) outlines the classical approach: qualities opposite to Vata’s nature. Warmth against cold. Moisture against dryness. Heaviness against lightness. Stability against mobility. Routine against irregularity. This translates into practical guidance: warm food and drinks, oil application to the skin and joints, regular sleep and meal times, avoidance of excessive sensory stimulation, and protection from cold and wind. The principle is elegant: you do not fight Vata, you give it what it lacks.
Abhyanga — therapeutic oil massage — deserves special mention because it addresses chronic pain through multiple pathways simultaneously. Oil is the direct antagonist of Vata: heavy, warm, smooth, and stable where Vata is light, cold, rough, and mobile. Applied to the skin (which is Vata’s primary seat), oil pacifies Vata at its home base. The warmth of the oil opens channels. The pressure of massage moves stagnant Vata and Ama. The nourishing quality of the oil supports depleted tissues. Abhyanga is not a luxury or a relaxation technique in the Ayurvedic context — it is a therapeutic intervention with specific physiological effects on the doshic and channel systems.
Panchakarma — the classical Ayurvedic purification therapies — plays a significant role in chronic pain that has not responded to dietary and lifestyle modifications alone. When Ama is deeply lodged in tissues and channels, it may require more intensive clearing than diet alone can provide. The specific Panchakarma procedures selected depend on the dosha pattern, the tissues involved, and the patient’s overall strength and constitution. For more on the principles underlying these purification therapies, see our article on Panchakarma.
Consider this: the body does not experience pain only where tissue is damaged. Referred pain — where injury in one location produces pain in a completely different area — is one of medicine’s most well-documented phenomena. A heart attack produces left arm and jaw pain. Gallbladder inflammation causes right shoulder pain. Kidney issues manifest as lower back pain. The pain is real, but it is not where the problem is. Ayurveda’s channel-based model (Srotas) provides an elegant explanation: the channels are interconnected, and a blockage at any point affects everything downstream. When a practitioner identifies the Srotas involvement rather than focusing only on the pain site, they are addressing the same reality that referred pain demonstrates — the body is a connected system, and where you feel the problem is not always where the problem lives.
Did You Know?
In 2011, neuroscientist A. Vania Apkarian at Northwestern University published a finding that stunned the pain research community: chronic back pain physically shrinks the brain. Patients with persistent pain for over a year showed a measurable reduction in grey matter volume — specifically in the prefrontal cortex and thalamus, areas governing decision-making, emotional regulation, and sensory integration. The longer the pain had persisted, the greater the brain loss. But here is the truly remarkable part: when pain was effectively addressed and reduced, the grey matter began to regrow. The brain damage was reversible. Ayurveda’s concept of Majja Kshaya — depletion of nerve and marrow tissue as a consequence of chronic Vata aggravation — maps onto this finding with uncomfortable precision. The classical texts described chronic pain not just as a sensation but as a progressive depletion of the nervous tissue that processes it. Pain does not just hurt. Left unaddressed, it physically diminishes the organ responsible for experiencing it.

What Current Evidence Says
Modern pain neuroscience has arrived at a concept called central sensitisation — the idea that in chronic pain, the nervous system itself becomes hypersensitive, amplifying pain signals and sometimes generating pain even without peripheral input. This is why scans can look “normal” while the person is in genuine agony — the problem has moved from the tissues to the nervous system itself. This parallels the Ayurvedic Vata-Srotas model remarkably: Vata (the nervous system force) becoming vitiated in Srotas (channels) to the point where the system perpetuates pain independently of the original cause. A 2023 study published in Nature Reviews Neuroscience confirmed that chronic pain involves measurable changes in brain structure and neural connectivity — it is as physically real as a broken bone, even when imaging of the painful area shows nothing. Both ancient and modern frameworks now agree: chronic pain is a fundamentally different phenomenon from acute pain, requiring different approaches.
Anti-inflammatory diets have been studied extensively for chronic pain management. A 2021 systematic review in the Journal of Clinical Medicine found that dietary patterns rich in whole grains, vegetables, fruits, and healthy fats — and low in processed food, refined sugar, and excessive red meat — were associated with reduced inflammatory markers and improved pain outcomes. This is consistent with the Ayurvedic emphasis on Sattvic, freshly prepared food and the reduction of Ama-producing dietary patterns.
Massage therapy for musculoskeletal pain has a substantial evidence base. A Cochrane review found moderate-quality evidence that massage therapy provides short-term relief for chronic low back pain, and the American College of Physicians includes massage among its recommended non-pharmacological therapies for chronic pain. The WHO’s Traditional Medicine Strategy 2014–2023 recognises Ayurveda as a comprehensive traditional medicine system and supports its integration into national health systems where appropriate. The mind-body connection in pain — now well-established in pain psychology — supports the Ayurvedic principle of Manas-Sharira inseparability: that emotional state directly influences pain perception and that addressing the mind is inseparable from addressing the body.
Chronic pain requires proper medical evaluation to identify or rule out underlying conditions that may need specific medical or surgical intervention. This article is for educational purposes only and does not constitute medical advice. Ayurvedic consultation can be a meaningful complement to your care, but should not replace medical diagnosis for pain of unknown origin, sudden onset pain, pain with neurological symptoms, or pain following injury. Always consult a qualified healthcare provider for persistent pain conditions.
